Real-time Eligibility Inquiry
CharmHealth uses the Clearinghouse service to get the Patient's insurance eligibility information from the Payer in real time.
Check Insurance Eligibility
From Patient Dashboard
- For the Practices enabled with this feature, the 'Check Eligibility' option will be enabled under the 'More Options' (...) icon in the Patient's Dashboard.

- Clicking on this option navigates the user to the 'Insurance Eligibility' view.
- Select the Patient's insurance, Provider, Service Type, and Date of Service to complete the eligibility check.

- Add Insurance & Edit Insurance - Options to Add new Insurance and Edit the selected Insurance are provided on this page.
- Insurance - All the Insurances added for this Patient get listed in the Insurance drop-down. The Payer name is shown along with the 'Eligibility Supported' or 'Eligibility Not Supported' text. This additional text indicates whether the eligibility check is supported for this Payer or not.
- Provider- The Providers list shows all the Providers and Facilities in the Practice. Refer to the 'Insurance Eligibility Settings' section to learn more about configuring the default Service Provider.

- Service Type - The Service Type field lists all the service types supported by the Payer. Refer to the 'Insurance Eligibility Settings' section to learn more about configuring the default ServiceType.

- The Patient details on the right-hand side will be sent with the eligibility request. Using these details, the Payer will search their database for the Patient's Insurance. Some Payers need additional details of the Patient such as SSN, Medicare ID, etc.
- Click on the 'Check Eligibility' button after selecting the appropriate details. CharmHealth sends an eligibility request to the Payer via your subscribed Clearinghouse and renders the response in a readable format. The eligibility information is separated based on the service type code in the response received. Select the service type code to view the eligibility details for the specific service type.

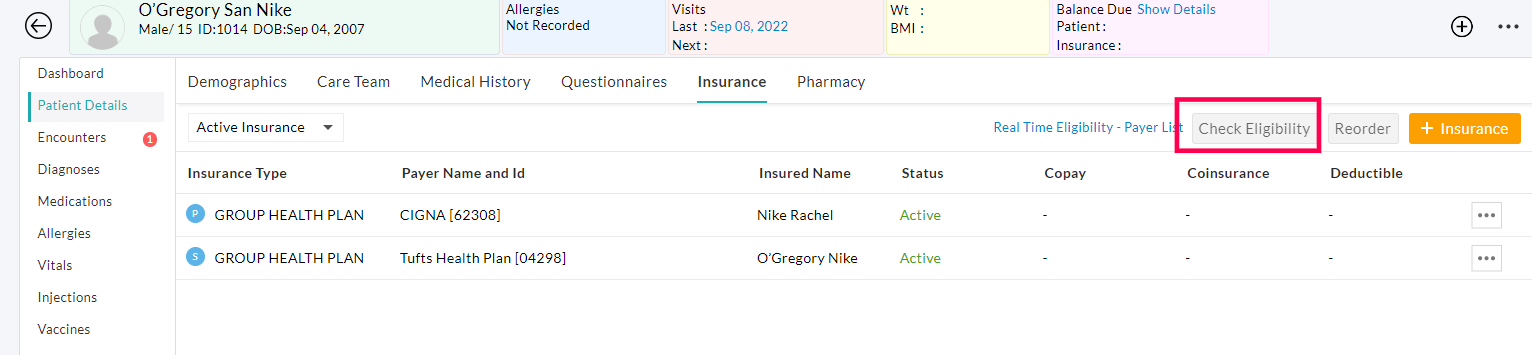
From Patient Dashboard - Insurance section
The 'Insurance Eligibility' option is provided in the Patient's insurance section as well. Refer to the below screenshot.

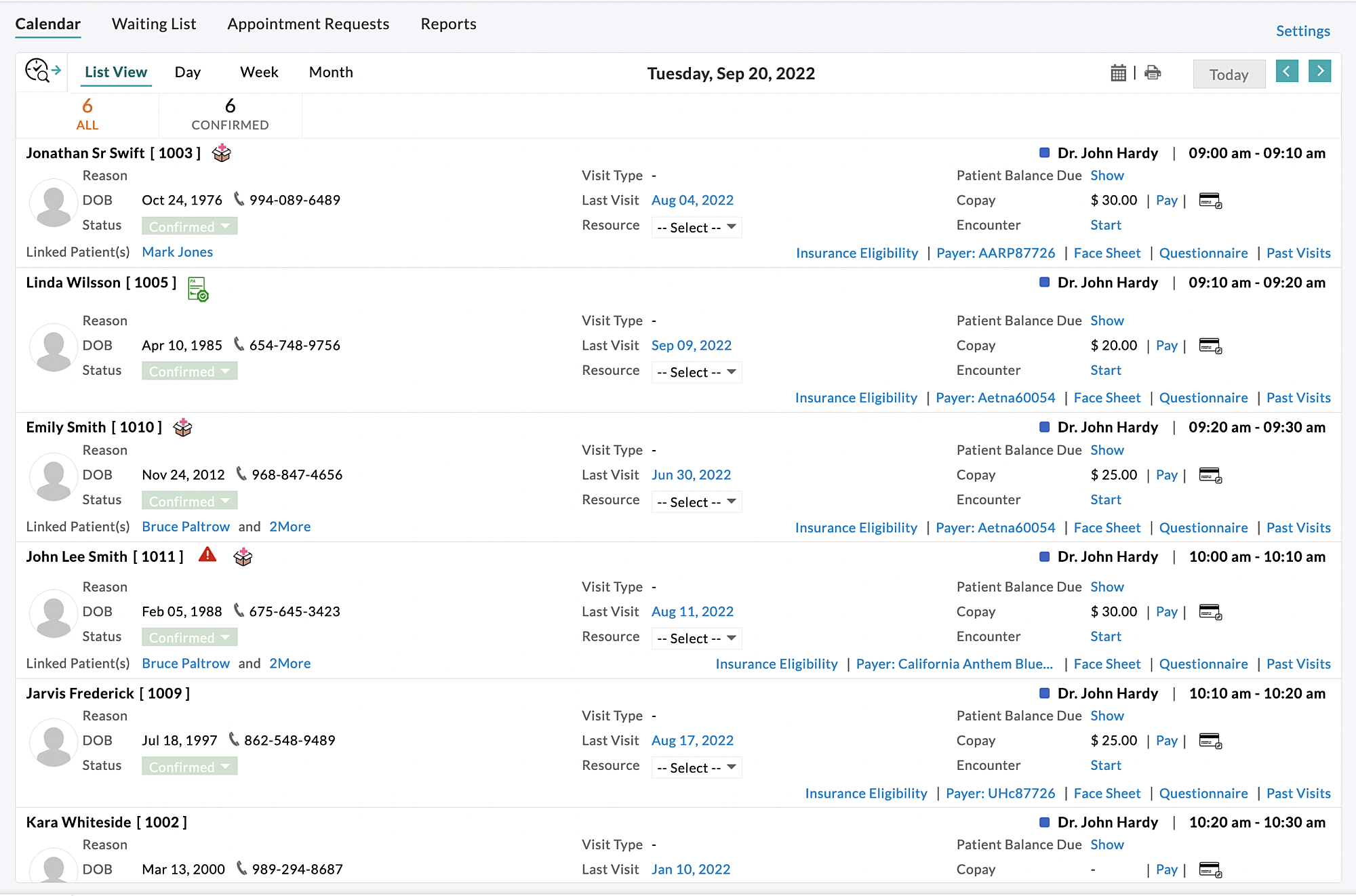
From Calendar - Appointment List View
The 'Insurance Eligibility' option is also provided in the Appointment list view for easy verification of the eligibility details by the Front office.
Insurance Eligibility History of a Patient
- The eligibility benefit information is stored and can be accessed in the future. To access the past eligibility details, click on the 'Eligibility History' option.

- All the past eligibility benefit details get listed in chronological order. Selecting any past eligibility request from the list will show the respective eligibility details.

Insurance Eligibility Settings
Practices can configure default preferences for performing real-time eligibility inquiries in this section. Both the global settings and Payer-specific rules can be defined to control how eligibility checks are performed for different Payers.
Navigate to 'Settings > Billing-eClaims > Real Time Eligibility Settings' and configure the following settings.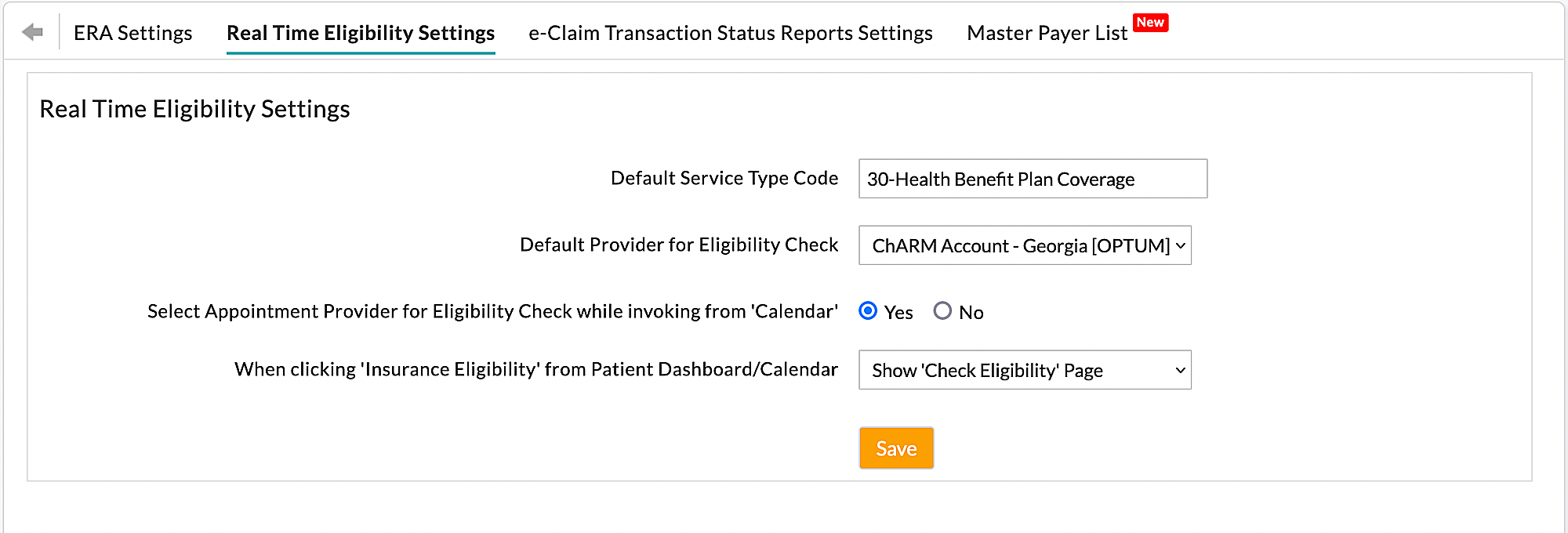
1. Default Service Type Code for Eligibility Request (270)
Select the default Service Type Code to be selected automatically while sending the Eligibility Request (270) to the Payer. The Service Type code used in the request (270) determines which type of benefits (e.g., Urgent Care, Health Benefit Plan) the Payer should evaluate for every eligibility request.
2. Default Provider for Eligibility Check
Select the Provider to be automatically chosen when checking eligibility from the Patient Dashboard or Calendar.
Furthermore, you can utilize the 'Appointment Provider' for eligibility inquiries related to Calendar appointments.
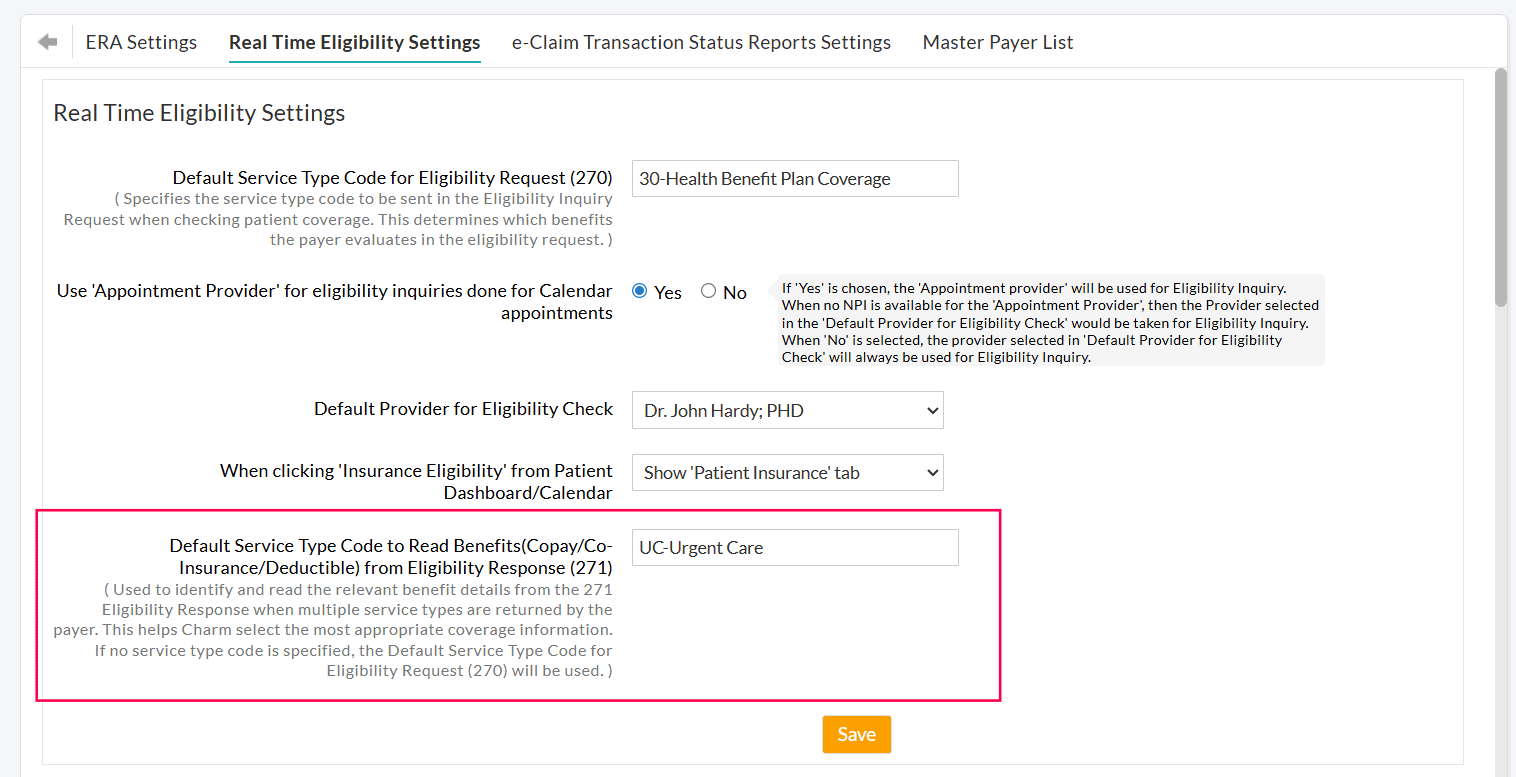
3. Default Service Type Code to Read Benefits from Eligibility Response (271)
Practices can configure a Default Service Type Code to read benefit details from the 271 response. This setting allows the Practices to define different Service Type Codes when sending eligibility requests (270) and when reading the responses (270), ensuring that the system returns accurate benefit details for your Specialty.
When the Eligibility Inquiry is done, some Payers may reject eligibility requests when the Service Type Code is not supported. To avoid this, Practices often use Service Type Code 30 (Health Benefit Plan Coverage), as it is widely accepted across Payers.
However, the eligibility response (271) typically includes benefit details for multiple supported service types, not just Code 30.
Since the details such as Copay, Co-insurance, and Deductible are service-specific, relying solely on Code 30 may not always return the most accurate benefit information.
With this update, Practices can now configure a separate Default Service Type Code to Read Benefits (271).
This allows Practices to:
- Send a generic request to improve acceptance rates.
- Retrieve and display benefit details based on a more relevant, specialty-specific service type.
Practical Example
If a Practice verifies eligibility for a Patient scheduled for an Urgent Care visit:
- Request (270): The Practice sends the Service Type Code 30 to ensure the Payer accepts the eligibility inquiry.
- Response (271): The Payer returns benefit details for multiple service types, such as General (30), Office Visit (11), and Urgent Care (UC).
- Result: Since the Default Service Type Code to Read Benefits 271 is configured as UC, CharmHealth bypasses the general information and displays only the Urgent Care Copay and Deductible.
If the 271 field is left blank, the system will use the same Service Type Code sent in the initial request (270) to read and display the benefit from the response.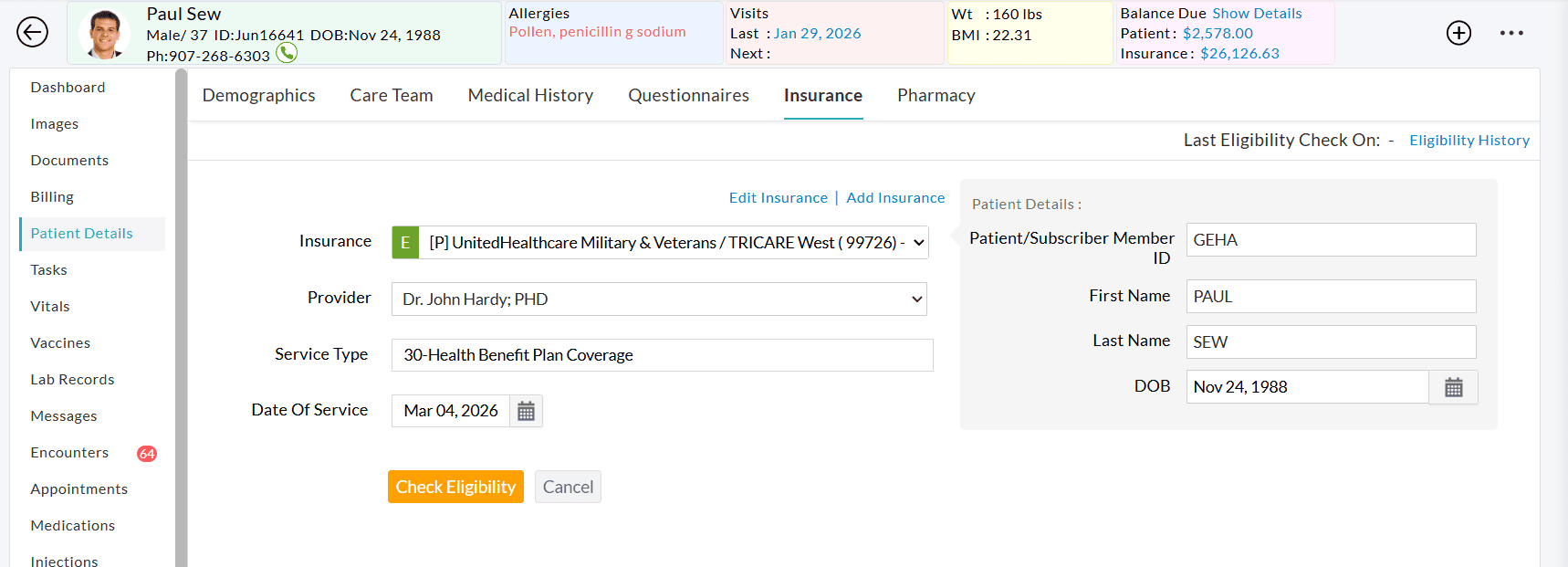
Payer-Specific Eligibility Settings
In addition to Practice-wide defaults, Practices can configure real-time eligibility settings for individual Payers, giving them the flexibility to define unique rules for specific Insurance Payers. This ensures that eligibility requests are tailored to the specific requirements of each Payer without impacting your global Practice defaults.
When an Eligibility check is initiated for a configured Payer, these custom settings automatically take precedence over the Practice-wide defaults. All other Payers will continue to follow the standard global configuration.
To configure,
- Navigate to 'Settings > Billing-eClaims > Real-Time Eligibility Settings > Payer-specific Settings'.
- Search and select the Payer you want to configure. You can search using the Payer name or the Eligibility Payer ID. If the Eligibility Payer ID is not available, the Payer ID will be shown.
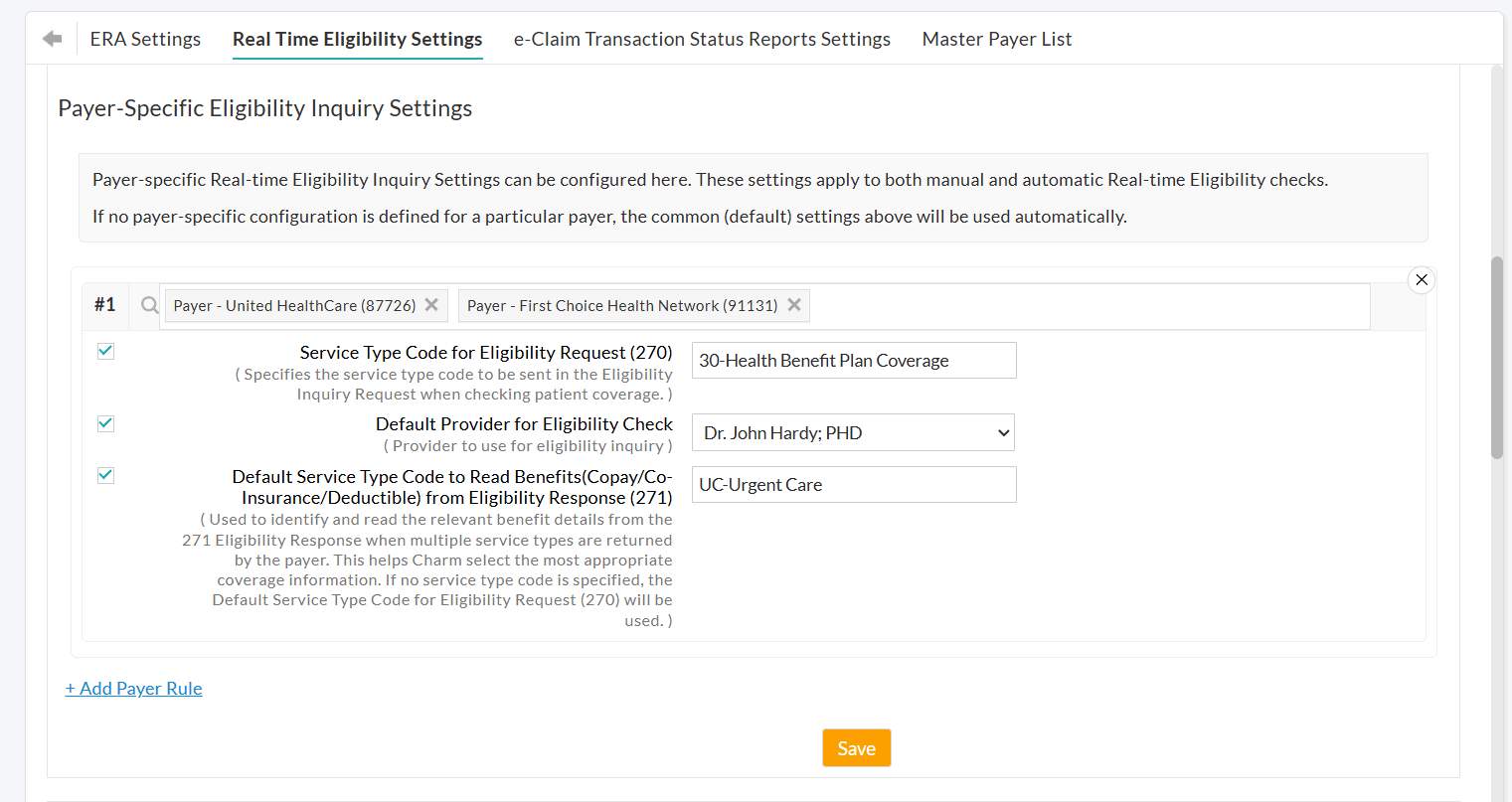
- Enable the required setting and enter the appropriate value for that Payer.
- Custom Service Type Codes: Set specific Service Type Codes for both the Eligibility Request (270) and the Eligibility Response (271) to ensure you receive and read the most accurate benefit details, such as Copay, Co-Insurance, and Deductible.
- Default Eligibility Providers: Designate a specific Default Provider for inquiries on a per-payer basis to satisfy unique Payer validation requirements.
- To add more Payer rules, click on the '+ Add Payer Rule' option.
- Save the settings.
Adding/Updating Eligibility Payer ID of the Patient's insurance
The list of Payers supporting real-time eligibility requests is available under the 'Settings > Billing-eClaims > Master Payer List' section. The Payers can be searched with the Payer Name or Payer ID, Eligibility Payer ID, or ERA Payer ID. If a Payer has a separate Payer ID for eligibility under the 'Eligibility Payer ID' column, then the same has to be entered under the 'Eligibility Payer ID' field while adding the Payer.
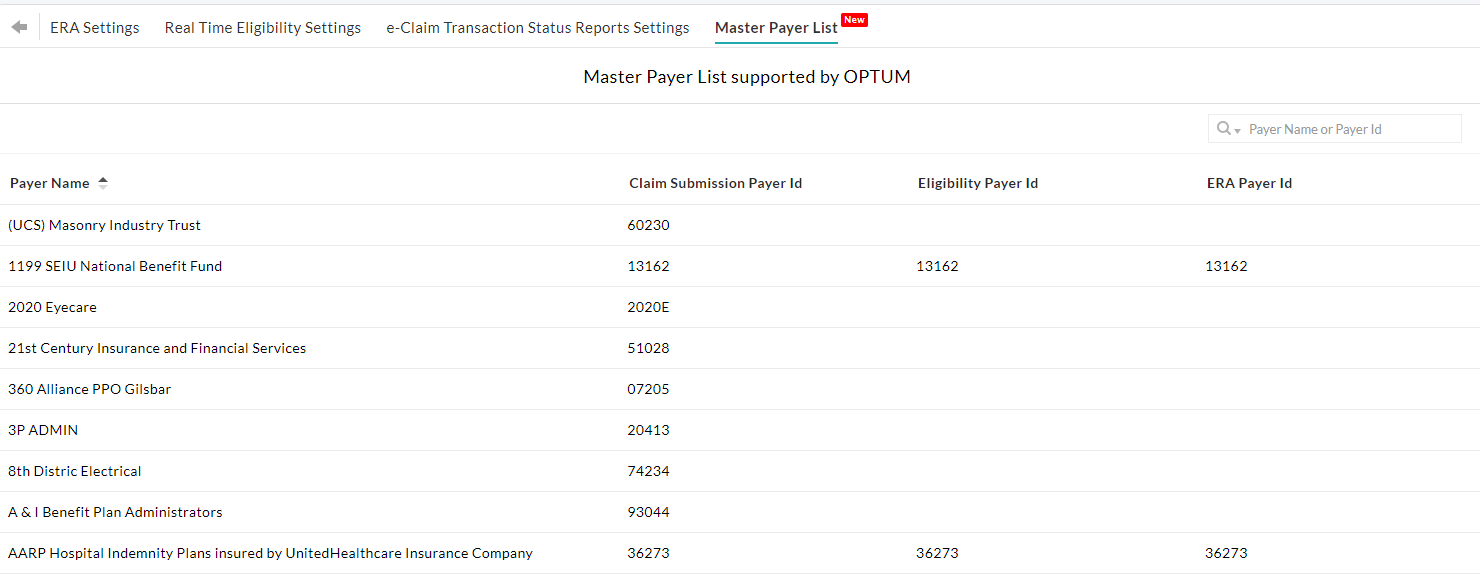
All payers added in the Practice are listed under the 'Settings > Billing - Claims > Payers'. In order to add/update the Eligibility Payer ID, click on the 'More Options' (...) icon against the payer, select the 'Edit' option,and update the Eligibility Payer ID.

Typical Error Messages
- Missing mandatory details: For each Payer, there are some mandatory details to complete the eligibility request. If the mandatory details are missing, CharmHealth prompts the user to enter the details.

Reason: This error indicates that the selected Provider/Facility doesn't have an NPI. NPI is mandatory to check Insurance Eligibility in real-time.
Solution: Navigate to 'Settings > Practice Members' List. Edit the respective Provider and update with a correct NPI. Similarly, if it is a Facility, then update the respective Facility under the 'Settings > Facilities' section. - Missing/Incorrect Information: The Clearinghouse will respond with the benefit information if there is any matching Insurance detail for the Patient. If not, the Clearinghouse responds with an error message. The following is one such error where the Patient's name and Date of Birth (DOB) in the demographics do not match with the Payer database.

Reason: This error indicates that the Payer could not identify the Patient with the given insurance details in their system.
Solution: Verify and update the Patient's insurance details with the correct DOB/Name/Member ID details. - Timeout Error: If CharmHealth does not receive a response from the Clearinghouse within 60 seconds, a timeout error will be shown. The users can send the eligibility request after a few minutes. Refer to the below screenshot.

Reason: The above error indicates that CharmHealth couldn't connect with Optum system to check eligibility.
Solution: Please try to check eligibility after some time.