AI-Powered Claim Validation and Suggestions
We are excited to introduce AI-Powered Claim Validation and Suggestions that provide intelligent, real-time guidance during Claim generation and editing. This feature helps billing teams proactively identify issues, improve Claim accuracy, and significantly reduce Payer denials before submission.
These suggestions are displayed in both the Preview and Edit Claim views.
Key Benefits
- Reduces Claim rejections and denials before submission
- Improves first-pass acceptance rates
- Saves time for the billing team by providing real-time support
- Ensures compliance with Payer-specific and CMS guidelines
- Provides clear, actionable feedback without disrupting the workflow
Intelligent Claim Analysis
Charm EHR performs a comprehensive analysis of the entire Claim, including:
- Procedure Code Validity
- Age Appropriateness Validation
- Gender Appropriateness Validation
- Modifiers Usage Validation
- Diagnosis and Procedure Compatibility
- Bundling and Unbundling
- Place of Service (POS) Consistency
This holistic evaluation ensures validations are context-aware and Payer-aligned.
Smart AI-Generated Suggestions
Based on the analysis, the system automatically generates actionable suggestions across key validation areas.
This includes the following:
- Procedure Code Validity
Detects invalid, inactive, or mismatched CPT/HCPCS codes. - Diagnosis & Procedure Compatibility
Ensures CPTs are clinically supported by the associated diagnosis codes.
Preview Claim View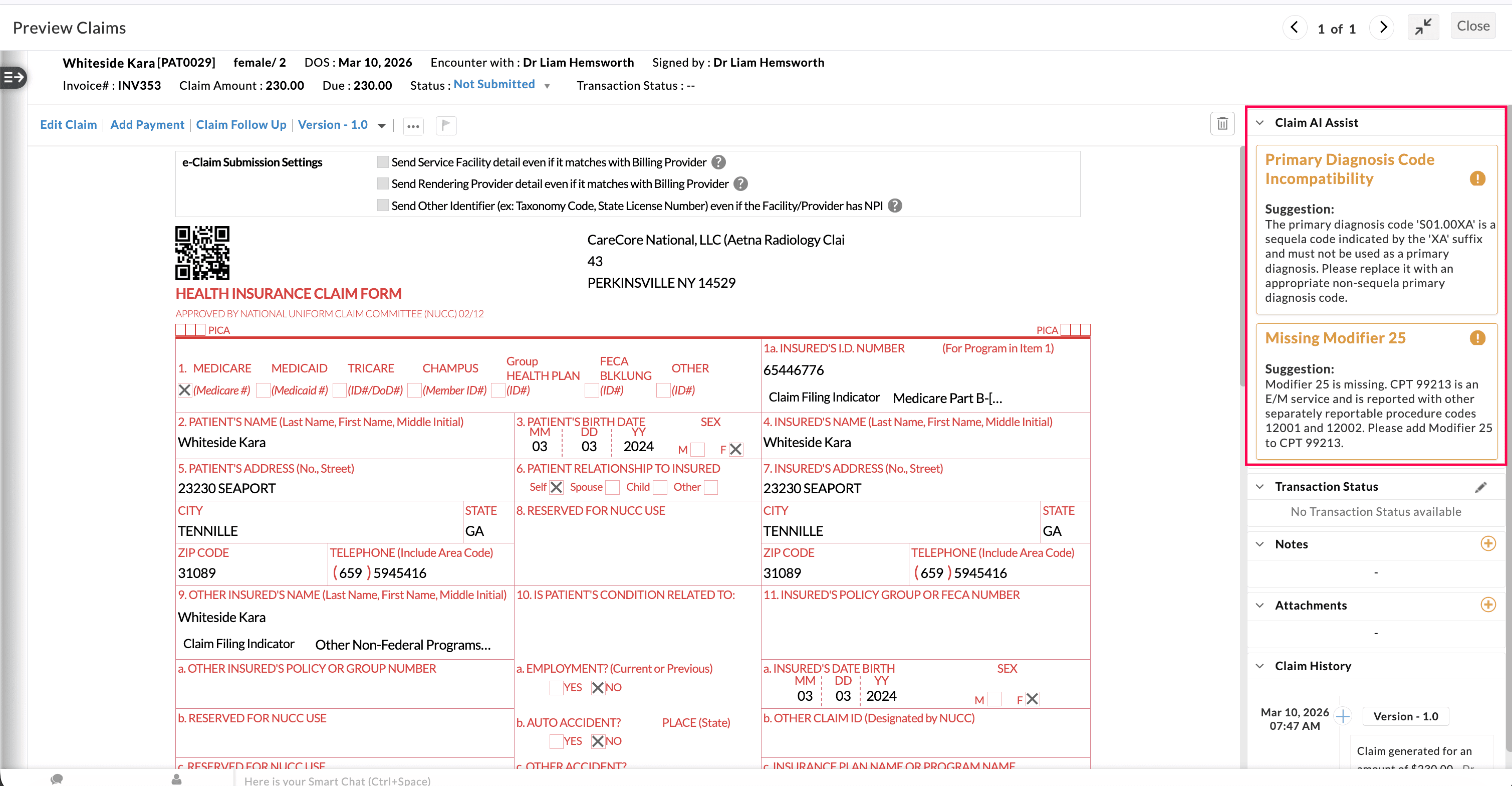
- Gender Appropriateness Validation
Identifies services that conflict with the Patient’s gender. - Modifiers Usage Validation
Validates correct usage, necessity, and compatibility of modifiers (e.g., 25, 59, TC/26). - Age Appropriateness Validation
Flags procedures or diagnoses that are not suitable for the Patient’s age.
- Bundling & Unbundling Checks
Detects incorrect unbundling or missing bundled components based on Payer rules. - Place of Service (POS) Consistency
Verifies alignment between POS, procedure codes, modifiers, and Provider/Facility type.
Automatic and Continuous Suggestions
- Suggestions are generated automatically during Claim creation—no manual trigger required.
- When a Claim is edited, the AI engine re-runs validations in real time and updates suggestions instantly based on the latest Claim details.
Edit Claim View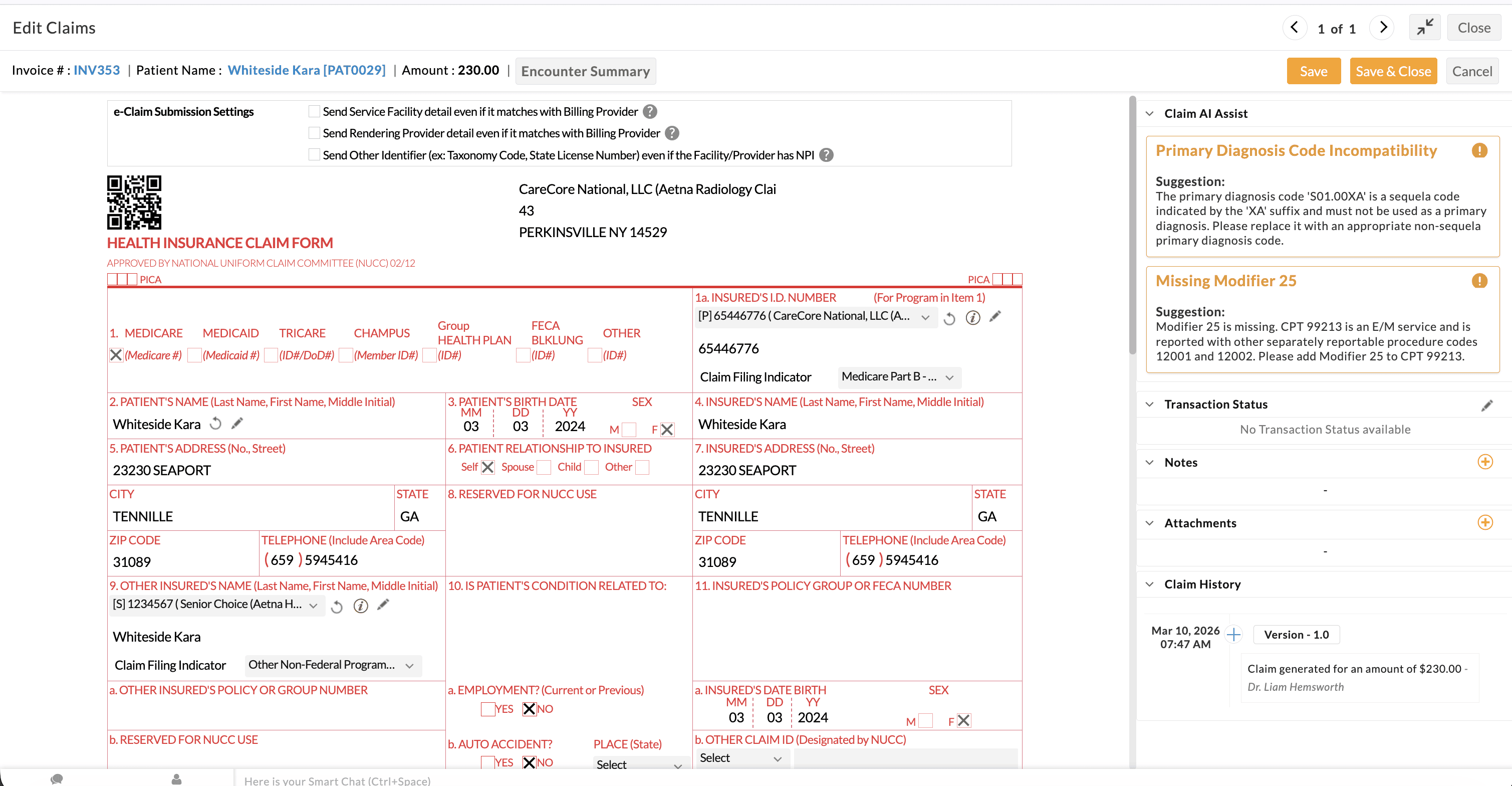
- Resolved issues are automatically removed, ensuring users see only relevant and current suggestions.